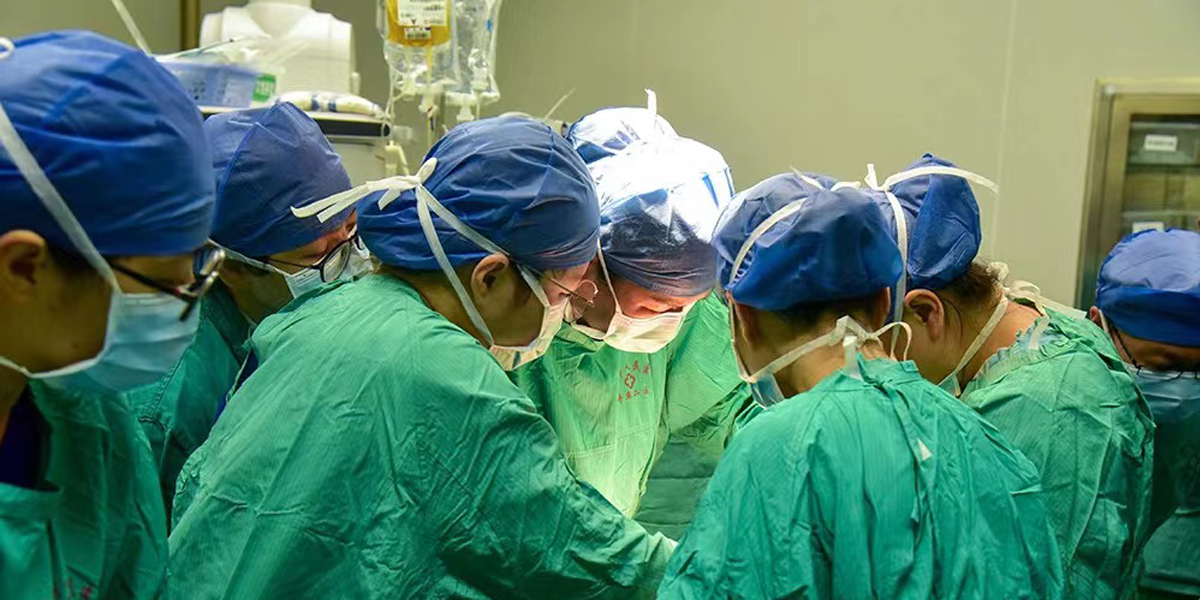
With the rapid development of surgical technology, surgical treatment has become the most important treatment method for surgical patients. Therefore, the operating room has also become the main battlefield for surgeons. The operating room is a department with a high risk of hospital infection and should be managed more intensively.
What is SSI in Surgical Terms?
Surgical site infections (SSIs) are defined as infections occurring up to 30 days after surgery (or up to one year after surgery in patients receiving implants) and affecting either the incision or deep tissue at the operation site. Particularly, SSI can sometimes be superficial infections involving the skin only.
Source: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4718372/
So, what prevention and control measures need to be implemented in the operating room to prevent surgical site infections?
Here are the most important 10 aspects:
1. Operating Theatre Staffs and Their Wearing
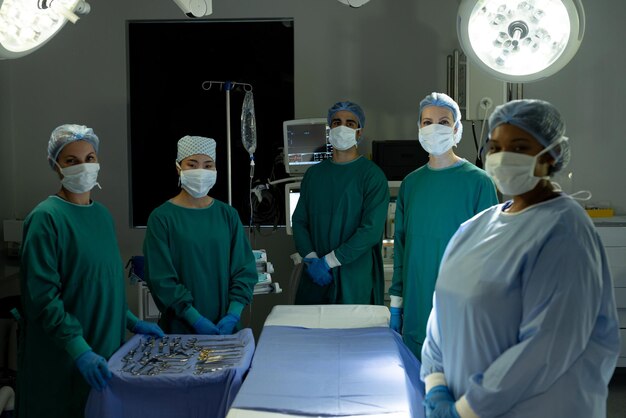
* Uniforms for Operating Theatre:
Standardized dress code: All operating theatre staff should wear the operating theatre-specific scrubs and working shoes, wear working caps and lace-up medical-surgical masks according to the procedure, and it is recommended that they wear disposable working caps, if they are cloth caps, they should be changed and sterilized every day. When going out temporarily, it is necessary to change shoes and clothes, and it is forbidden to work in non-operating theatres with scrubs. (Surgical Gowns of All Levels: https://www.tecbodmed.com/surgical-gowns_c14 )
* Prohibited Wearing:
Earrings, rings, bracelets, and other ornaments should be removed before changing, nails should be trimmed and false nails are prohibited.
* Quantity of Staff:
Strictly control the number of personnel entering the operating theatre, unrelated personnel are not allowed to enter; observation personnel should obtain permission from the person in charge of the operating theatre and then arrange for a special person to guide them to enter. During the operation, all personnel should be minimized the number of times they enter and leave the operating theatre, and keep the door of the operating theatre closed.
* Prohibition of Participation in Surgery:
Healthcare workers suffering from acute upper respiratory tract infections, infectious diarrhea, skin boils, carbuncles, and other infectious diseases should not participate in the surgery.
* Strengthen the Management of Medical Device Representatives:
Non-mandatory device dealers should not be set up as followers, and when it is necessary to follow them, they should be trained in advance on infection prevention and control, and their concept of asepsis and aseptic operation should be supervised and guided throughout the whole process.
2. Disinfection
* Unsterile Team Members
Includes anaesthesiologist, circulator, biomedical technicians, radiology Technicians or Other Staff that might be needed to set up and operate specialized equipment or devices essential in monitoring the patient during a surgical operation) should strictly carry out the hand disinfection process under the 3B & 4A below:
- Before contact with the patient
- Before access to sterile items
- Before aseptic manipulation
- After contact with the patient
- After contact with the patient's surroundings
- After contact with blood and body fluids
- After removal of gloves
* Sterile Team Members
Includes Surgeon, Assistants to the surgeon, Scrub person (either a registered nurse or surgical technologist) should strictly follow the surgical hand disinfection process to ensure 100% compliance and correctness of surgical hand disinfection.
* Operation Theatre Quality Surveillance Team
Surgical hand disinfection should be included in the daily quality control of the department by regularly accessing the hand brushing area to monitor and supervise and check the surgical hand disinfection of the participating surgical staff.
3. Strict Asepsis
* Pre-service Training
All staff entering the operating theatre, including surgeons, advanced trainees, and interns, should undergo theoretical and skills training and assessment on relevant knowledge of infection prevention and control, the concept of asepsis, surgical hand disinfection, and aseptic operation.
* Strict Enforcement
All surgical staff must strictly enforce surgical hand disinfection by correctly wearing sterile gowns and sterile surgical gloves (contact-free gloving is promoted). When everything is ready, the back, below the waist and above the shoulders are regarded as sterile areas and must not be touched with hands. Passing objects and changing positions correctly, do not pass instruments and objects from behind or above the head of the surgical staff; if the surgical staff on the same side need to change positions, they should take one step backward and turn to another position back to back to prevent touching the unclean area on the other side's back. Before incision of cavity organs, gauze pads or incision protectors should be used to protect the surrounding tissues; intraoperative contaminated instruments should be put into the tray dedicated to contaminated instruments; resected specimens should be passed by contactless delivery, and it is prohibited to pick up with bare hands; after completing all the steps of contamination, the surgical staff should change the sterile surgical gloves before they can continue the operation.
*Mutual Supervision
All staff in the operating theatre should supervise each other and remind each other that the observers should be more than 30cm away from the operator, and the height of the footstools should not be more than 50cm. when the personnel on the operating theatre need to ask for help in wiping off the sweat, their heads should be turned to the other side.
4. Environmental Management of the Operating Theatre
* Monitoring of the Temperature, Humidity, and Pressure Difference:
Daily monitoring of the operating room temperature, humidity, and differential pressure will help to ensure that within the normal range, found abnormal, timely repair, timely search for the cause, rectification, timely improvement of monitoring and maintenance records.
* Strictly Daily Disinfection
Cleaning up and disinfection to the operating room environment very day before the start of surgery and after the end of surgery promptly do a good job of , pick up the table between the surgery, should be cleaned and disinfect the operating table and the surrounding surface of the objects within the range of 1 ~ 1.5, contamination at any time to clean and disinfect. Purification of the operating room is to be strictly to the requirements of the completion of the operating room self-cleaning.
* Weekly Cleaning
The operating room, sterile storage room, liquid room, anesthesia recovery room, instrument and equipment staging room, and other auxiliary rooms should be thoroughly wet and wiped to keep clean weekly.